We’re not asking for anything extra — just to stop Chester going through unnecessary trauma during an already tough cancer journey
We wanted to share what’s been going on behind the scenes around Chester’s NG (nasogastric) tube — not because we like to complain, but because what we’ve experienced has been really frustrating, and it’s caused unnecessary distress for Chester. If it’s happening to us, it’s probably happening to other families too!
Chester has a long-term NG tube as part of his treatment. These tubes are designed to stay in place for around 90 days, according to both NHS guidelines and manufacturer advice. After that, they’re meant to be replaced — not just because of the guideline, but because they physically break down over time, irritate the lining of the stomach, and cause damage to the skin on the cheek where the dressing sits.
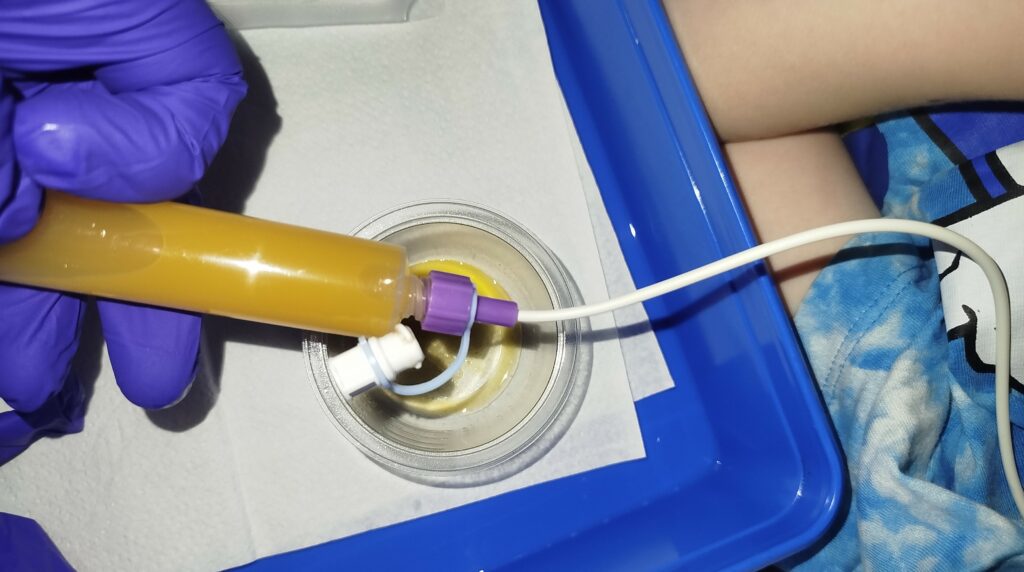
In Chester’s case, all of that has happened. One tube caused bleeding from his stomach. Two others broke completely after 3-4 months. Another came out when he was sick and was completely degraded — it looked horrific. And the longer a tube stays in, the more it rips and damages his skin under the dressing. When the tube is finally changed, it’s often raw, red, and painful, which is why we’ve always tried to plan ahead and tie any NG tube changes in with his LPs (lumbar punctures), which are always done under general anaesthetic. That way, he’s asleep, and there’s no trauma. It’s what we were told we could do from the start — not routinely, but if it helped avoid distress.
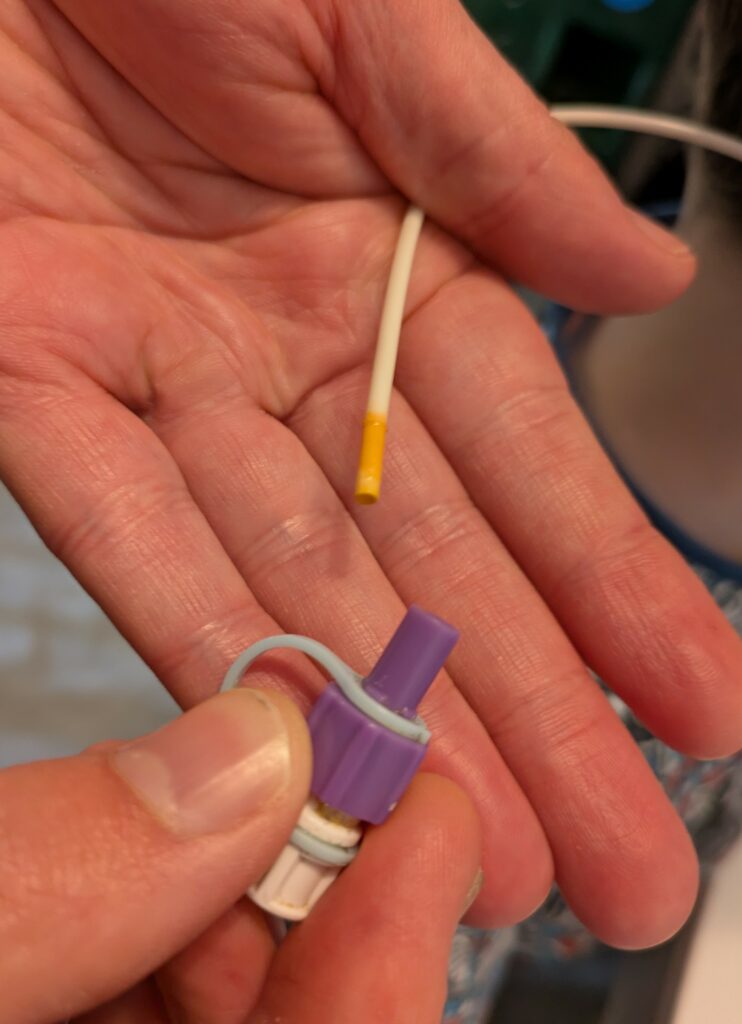
But recently, something changed — and no one told us.
When we asked at his LP in April for the NG to be changed (it had been in more than 3 months at that point), we were told no, unless it was physically damaged. We explained why we were worried — we didn’t want it to break like all the other times, and end up needing an awake change. Unfortunately, that’s exactly what happened. It broke a few weeks later, and Chester had to have it done at home, fully awake. We had to hold him down. He didn’t speak to us for two days afterwards. It was horrible for him and us.
We were also told that the 90-day replacement timeline is now just a “guideline to work with,” and that NG tubes aren’t routinely changed anymore unless they’re physically damaged. But in practice, that means they’re willing to leave the tube in for as long as possible, regardless of the impact on Chester’s skin or the risk of it breaking. Just because it looks okay on the outside doesn’t mean it’s not degrading or causing harm on the inside. We’re not asking for it to be changed the moment it hits 90 days, but waiting until it fails isn’t safe or fair. We’re just trying to prevent distress, not respond to it after the fact.
When it broke last time, we even tried to tape the end with medical tape to keep it going just a little longer — but it wouldn’t hold. It was completely degraded, and there was no safe way to keep it in. We did everything we could to avoid putting Chester through an awake change, but in the end, we had no choice.

Chester has had to go through a few awake NG tube changes before, and every time, it’s been horrible. The first was right at the start of treatment when he stopped taking his oral meds, and he had to have a tube put in. Others have happened when he’s been sick and the tube’s accidentally come out. We completely understand that sometimes it has to be done, but for Chester, it’s not just a quick procedure. He says it’s really painful, even though some nurses tell him “it won’t hurt.” But how would they know? It’s not their body. Afterwards, he won’t speak to us for days, and it’s incredibly hard seeing him go through that.
He has to be pinned down, often in front of his sisters — it’s traumatic for him and for all of us.
But we asked for it to be changed because his lumbar punctures are no longer every other week or monthly — they’re now more spaced out, so we knew the tube would be in for longer periods and his skin would become very sore. We were, again, just trying to plan ahead. But they refused to do it, and it ended up causing Chester a lot of distress.
We’re already going through the most stressful time of our lives — watching our child go through cancer treatment, hoping everything goes smoothly each time. On the day of an LP, there’s already so much going on. We’re asked to confirm his chemotherapy, sign paperwork, answer medical questions, and flag any concerns. It’s a lot. And now, on top of all that, we have the added worry of whether his NG tube will be changed — something that should be straightforward. We’ll probably have to keep bringing it up ourselves, just in case it’s forgotten, like other things have been in the past. It’s yet another emotional burden during an already heavy day.
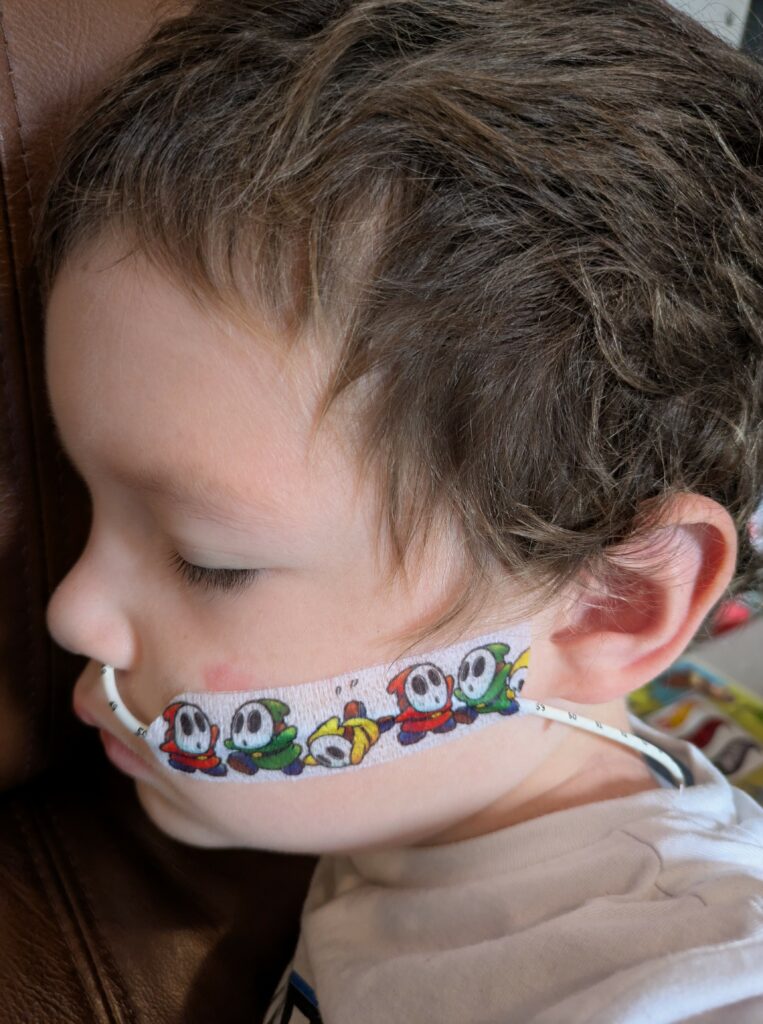
After that, we sent several emails to try and get clarity. We asked the matron directly. We chased through our community nurse. We were told vague things like “we’ll escalate it,” or “it needs pre-planning,” or “it depends on the anaesthetist on the day.” No one will actually confirm if it will be done at the next LP in September — even though by then, the tube would have been in for over 3 months, and the LP after that wouldn’t be for another 3 months, meaning the tube could end up being left in for over 6 months, with his skin becoming increasingly sore. That’s if it even lasts that long. We explained clearly how distressing it is for Chester — and that it’s not just about guidelines, it’s about what he’s actually been through — but we never got a proper response. Even our last email to the matron went completely ignored.
Our community nurses contacted them too, as she knows how traumatic this is for Chester. She told them tubes should be changed every 90 days, and that changing it during LP is the kindest and least distressing option. But she was also met with the same response: it’s no longer routine, guidelines have changed, and they won’t guarantee it can be done.

At Chester’s most recent LP on 17th July, we still went in not knowing what the actual rules are. One of the CNS nurses confirmed that NG changes are no longer done routinely and won’t be done just for distress or mental health reasons — because it’s a procedure that “can be done at home.” She said she’d put Chester down for a change at his next LP but was clear: there are no guarantees. It would depend entirely on which anaesthetist is on the day and whether they agree to do it.
That’s when she confirmed what we’d suspected: the real reason is time.
Their LP lists have become much busier, and they’ve been told not to do anything “extra” unless absolutely necessary. Even though changing an NG takes just two minutes — even if the child is already under — they’re told not to do it unless the tube is physically broken.
So even if the tube is nearly six months old, causing sore skin, and unlikely to last another three months, it might still be left. That just doesn’t feel fair — especially when we’re not asking for anything new or unreasonable. We’re simply trying to avoid another traumatic awake change. It’s not Chester’s fault the list is busier, and he shouldn’t be the one to suffer because of it.
Also, we’ve always pre-warned Chester a few days before his “sleepy test” (as we call it) if he might be having his NG tube changed. It gives us time to prepare him gently — we play little games to distract him, talk about it calmly, and let him know what to expect. He also likes to choose what tape he’ll have next, which gives him a small bit of control over something that otherwise feels very out of his hands. Knowing what’s coming helps him feel safer, and he’s usually okay with it as long as he’s had time to process it.
Even though having the tube changed under anaesthetic is far less distressing than being awake, it’s still a big change for him. When he wakes up, the tube is on the other side, and that unfamiliar feeling really throws him. Especially when he’s on steroids — tired, hungry, emotional — he often wakes up moaning or disoriented, overwhelmed by the change. That’s why preparing him in advance is so important. But now, we’re not even able to do that — because it’s all left to chance. We don’t know whether to tell him or not. If we do and it doesn’t happen, he gets worked up for nothing. If we don’t and it does, he wakes up upset and confused. Either way, it’s unfair on him.
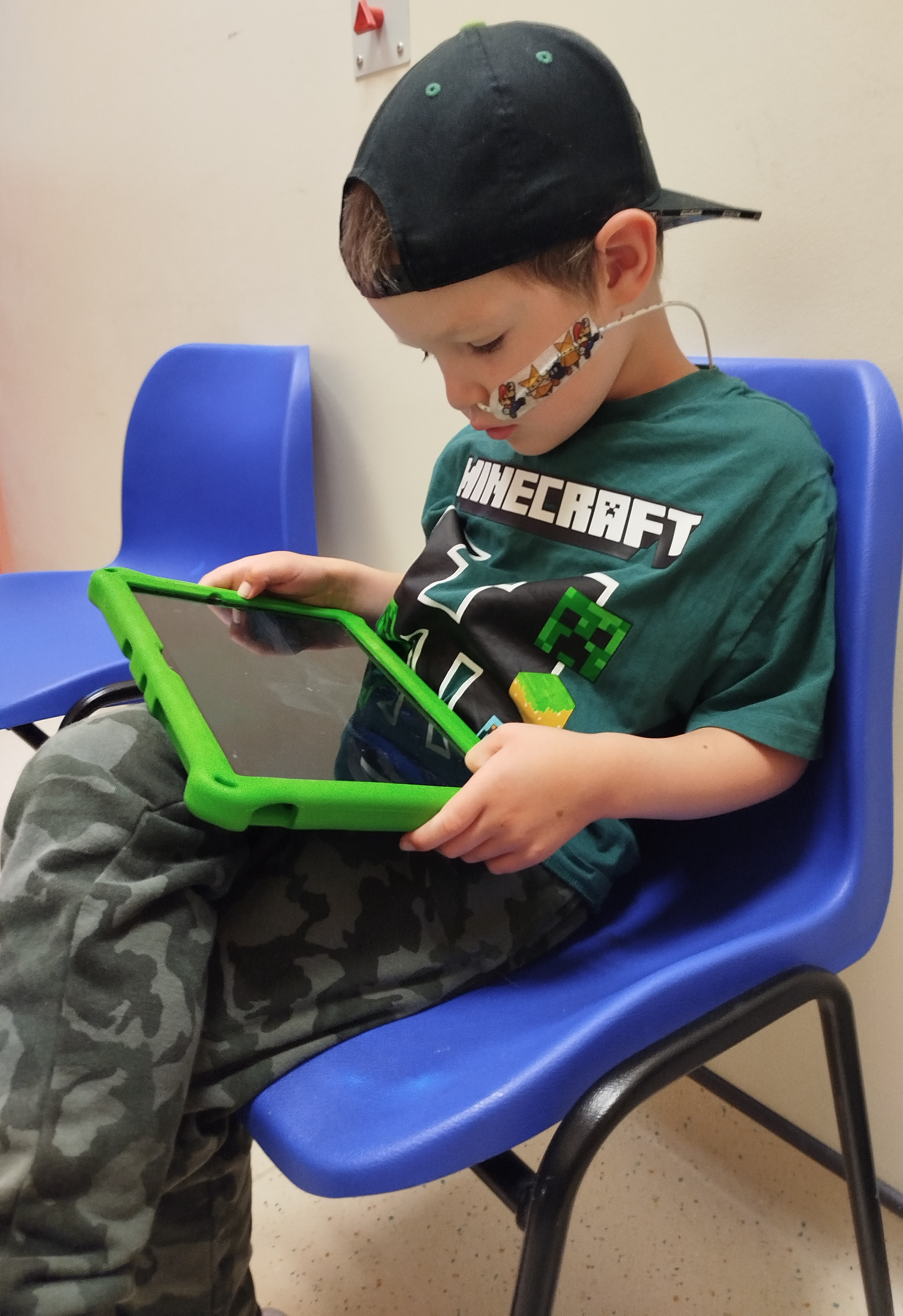
We also spoke to one of the consultants, who said that no, it’s not done routinely, but yes, in Chester’s case it should be done next time to help with skin breakdown and comfort and to avoid it breaking in the future.
We even mentioned the issue again today to a consultant at our local hospital, and when we said that the tube might not be changed again, her response was, “The Hospitals are very busy and under a lot of pressure — the list is very long now and it’s done across two days.” She was clearly just defending them. There was no acknowledgment of what this actually means for Chester — or for us as a family. It felt like the pressure on the hospital mattered more than the impact on a six-year-old going through treatment. We understand things are busy. But why should that mean children are left to suffer?
So we’re left feeling like we’ve had to fight for something that should be simple — a quick, two-minute task that could save a lot of pain. Instead, it’s being pushed aside as an inconvenience, and families like ours are left crossing our fingers and hoping that someone decides to care on the day.
What’s frustrating is that in the past, whenever we asked for the NG to be changed during his LP, it was done without issue. We were told it could be added if needed to avoid distress, and for a long time, that’s exactly what happened. But now, everything seems to have changed — and not for medical reasons, just time pressures.
We’ve also been told more than once that children on maintenance are “not as much of a priority,” and to be honest, it feels like that’s part of the problem too. There just isn’t the same level of care or attention anymore — like because Chester isn’t having chemo every week, he no longer matters quite as much.
And the truth is, we didn’t choose this for him. He didn’t choose to need chemotherapy or have Philadelphia-positive leukaemia, or to be unable to tolerate his medication. The NG tube wasn’t something we pushed for — it was suggested to us, and we were told it could be managed and changed while under sedation when needed. But now, suddenly, it’s a problem. Now it’s “not necessary” or “can be done at home,” simply because they don’t want to take two extra minutes to help avoid trauma for a child.
We’ll keep speaking up — not just for Chester, but for any other child who might be left in the same situation.

On top of all this, we can’t help but feel like Chester is sometimes treated like just a number — not a child who’s been through so much. It often feels like as long as the list gets done and the staff get to their lunch break, it doesn’t really matter if Chester is left distressed or uncomfortable. We’re asked to arrive at 8:30am every time, but consultants don’t arrive until around 9am, and the lumbar punctures never seem to start until closer to 10am — sometimes a bit earlier if they take inpatients first.
But despite being on time, we’re often left waiting for hours, and Chester’s name doesn’t come up until late morning or even early afternoon. We’ve been doing this for a long time now, and it’s a clear pattern.
Last time, Chester was on steroids — he was starving, thirsty, and understandably irritable — but even then, we overheard staff saying they weren’t aware he was on steroids, which is worrying, as steroid patients are supposed to be prioritised and seen first. It’s actually the second time this has happened. It makes us wonder how much of his care is truly being considered, or if he’s just seen as another slot on a busy list.
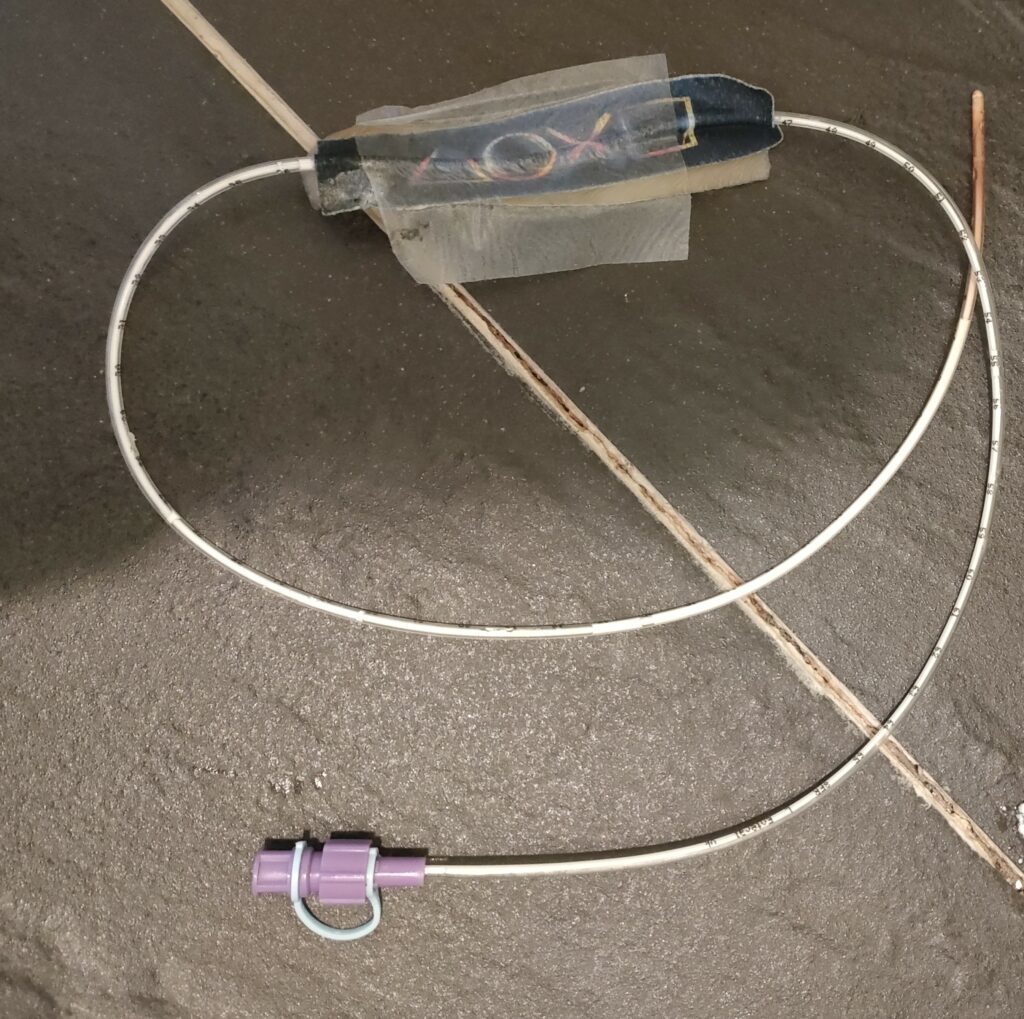
A Gentle Reminder: What the Manufacturer Recommends
It’s not that we’re demanding the tube be changed more often than the rules—far from it. The manufacturer’s leaflet is clear: these tubes are made for up to 90 days in place. Maybe other hospitals use a different brand of tube that can stay in even longer, and that’s fine for them. But for Chester, it’s not just about following a number. We’re asking for changes to happen in the safest, least traumatic way possible—ideally under sedation, during another planned procedure like his next lumbar puncture, just as it’s always been done before.
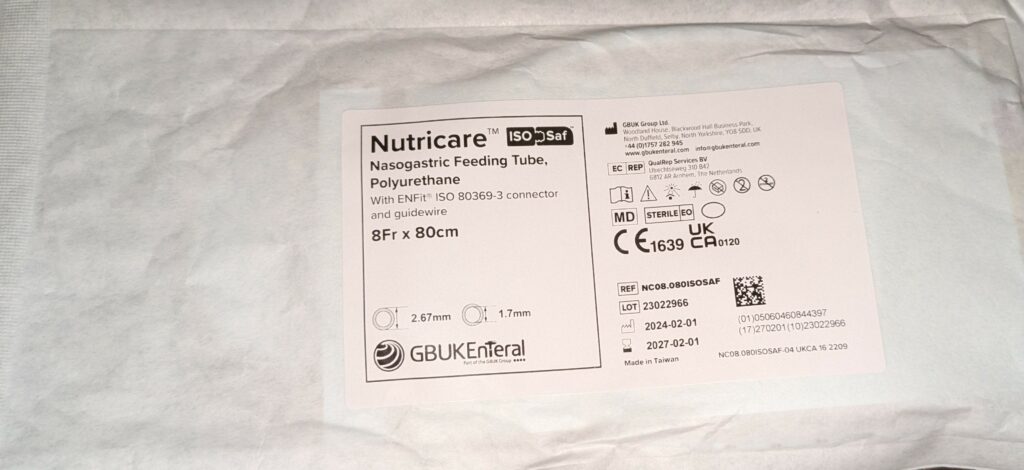
Yes, technically, they could change it at home while he’s awake. But for Chester, that causes enormous distress, and we’ve learned from experience it’s not worth it. This is about doing what’s kindest for him—following the guidance for the tube he actually has, and making decisions that put his wellbeing first. Is that really too much to ask?
And just so there’s no doubt, above is the picture of Chester’s actual tube and below is the page from the product brochure on the manufacturer’s website. You can see for yourself—it really does say ‘up to 90 days.’ But at the end of the day, it’s about listening to families, working together, and doing what’s best for each individual child.
